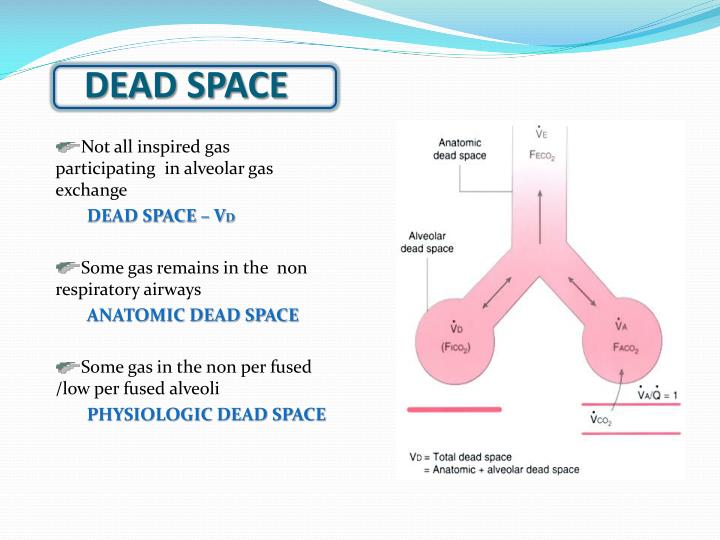
In contrast, hypoxemia that results from ventilating alveoli that have less ventilation than perfusion (ie, low ventilation-to-perfusion ratios as occur in asthma Asthma Asthma is a disease of diffuse airway inflammation caused by a variety of triggering stimuli resulting in partially or completely reversible bronchoconstriction. This effect ensures constant admixture of deoxygenated blood into the pulmonary vein and hence arterial hypoxemia. Whatever the cause of airspace filling in AHRF, flooded or collapsed airspaces allow no inspired gas to enter, so the blood perfusing those alveoli remains at the mixed venous oxygen content no matter how high the fractional inspired oxygen (FIO2). Later, there is proliferation of alveolar epithelium and fibrosis, constituting the fibro-proliferative phase. This early phase of ARDS is termed exudative. The airspace collapse more commonly occurs in dependent lung zones. In pulmonary hypertension, pulmonary vessels may become constricted. 
It has many secondary causes some cases are idiopathic. Edema fluid, protein, and cellular debris flood the airspaces and interstitium, causing disruption of surfactant, airspace collapse, ventilation-perfusion mismatch, shunting, and pulmonary hypertension Pulmonary Hypertension Pulmonary hypertension is increased pressure in the pulmonary circulation. These substances damage capillary endothelium and alveolar epithelium, disrupting the barriers between capillaries and airspaces. The cytokines activate alveolar macrophages and recruit neutrophils to the lungs, which in turn release leukotrienes, oxidants, platelet-activating factor, and proteases. In ARDS, pulmonary or systemic inflammation leads to release of cytokines and other proinflammatory molecules.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
